A 32-year-old newly transferred patient tells the medication nurse he sees blood in his urine. The nurse asked him to submit a sick call slip. Ten days later he is taken to the emergency room with flank pain and hematuria, having not yet been seen in sick call. A review of his chart indicated he was on a standing dose of 5mg of Coumadin (warfarin) without any INR orders since before the transfer from a facility two hours away.
Unfortunately, this is a snippet from an actual situation. It underscores the often disconnected nature of correctional health care and the need to have a well-established system to monitor the effects of high-risk medications like Coumadin (warfarin). The medication nurse had not made the connection between the patient’s bleeding and the medications she was administering. It is apparent that there are several patient safety issues here. What questions do you have about this case? Here are mine.
- Why did the nurse not connect bleeding with the patient’s medication profile?
- Did the patient follow through with submitting a sick call slip?
- How was the sick call request triaged? Why was bleeding not prioritized to be immediately scheduled for an evaluation?
- Why is Coumadin ordered without an INR order?
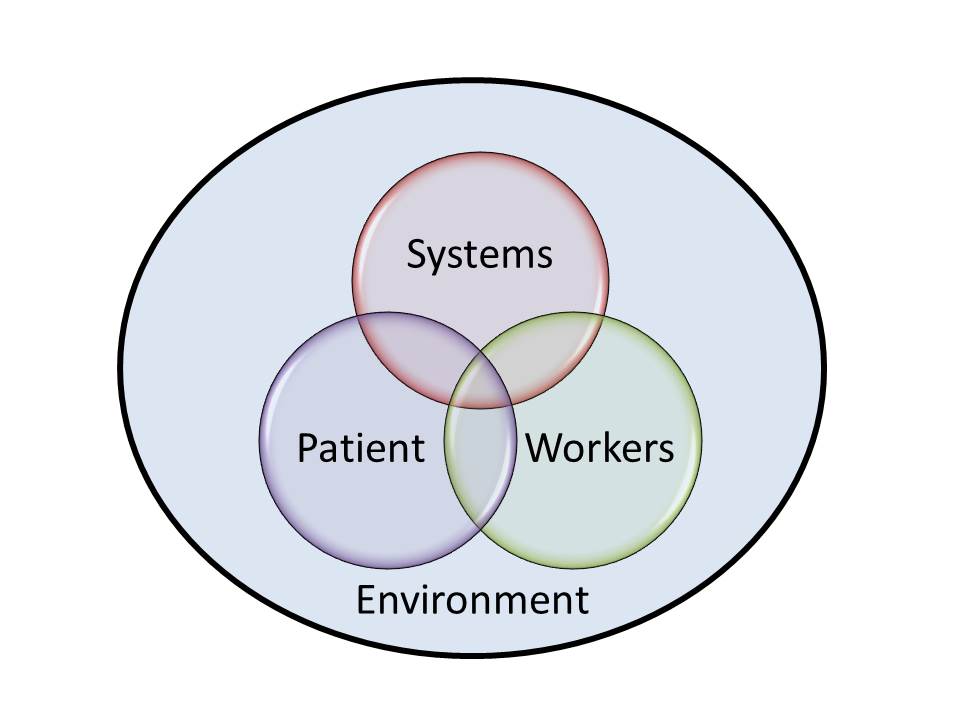
When I evaluate a patient safety issue such as this one, I will often use the 4-part model authored by my colleague, Lorry Schoenly, and detailed in her book, “The Correctional Health Care Patient Safety Handbook,” that takes into account the components of the care environment, the therapeutic systems, patient involvement, and the care givers in determining how to make improvements and learn from the experience. Let’s evaluate this situation from this four-fold evaluation of all possible elements.
Environment
The environment of care is both the physical environment and the organizational culture of the workplace. As you might imagine, this component is the most difficult to change in any setting. Correctional facilities are designed for security and not for health care delivery. Medication administration often takes place in the housing area or a location away from the medical unit, such as the dining hall or rec yard. The patient’s medical information, other than the MAR, is often unavailable.
The organizational culture is also based on security need rather than health care considerations. I have often said that correctional nursing is the only nursing specialty that works in an environment where healthcare is not the primary mission. Many times nurses are pressured to administer medication in an unreasonably short time period based on inmate movement and the security schedule. It is easy to develop tunnel-vision when 200 patients are scheduled for morning meds.
Systems
Standard systems for high-risk processes can reduce the chance of situations like the one described here. The therapeutic response to medications is often monitored during chronic care visits and this patient should have been on the roster for regular attention to his blood disorder. However, measuring therapeutic blood levels should be a standard part of every Coumadin (warfarin) medication order to decrease the chance of situations like this occurring. In fact, the following medications should be titrated based on blood levels:
- Anticoagulants (warfarin/heparin)
- Digoxin
- Dilantin
- Lithium
- Theophylline
Patient
In this case, the patient could have been a help in monitoring the medication effect. He was knowledgeable about his condition and initiated communication with health care staff about his concerns. Patients can be very helpful in reducing medication errors and improving monitoring efforts. See this prior post about ways your patient can help you avoid medication errors.
Care Givers
The staff member delivering medication at the point of care is the last checkpoint against error. In a chaotic work environment where health care tasks may be disjointed and fragmented, staff members can easily develop a task-based model of care. There are indications of this mindset in this case as the nurse directs the patient to drop a sick call slip rather than hearing the concern from the contact of the total patient situation. In addition, bleeding is a high-level concern, no matter the reason, and this patient needed immediate, rather than delayed, attention. Other caregiver concerns to explore include a lack of knowledge, cynicism, and fatigue.
Monitoring the effects of medication is a correctional nurse challenge, but nonetheless, an important aspect of medication administration. How do you deal with this in your setting? Share your tips in the comments section of this post.
Leave a Reply