In this post, we continue our discussion of Systemic Lupus Erythematosus.
Nursing Interventions for the Patient with Systemic Lupus Erythematosus
ASSESSMENT AND HISTORY
The importance of obtaining a detailed history from the patient, including present and past symptoms, and family history of autoimmune disorders, cannot be overstated. Medication history should also be solicited from any patient who presents with symptoms of SLE. A full physical examination should be done, and a referral should be made to a provider if results suggest the patient has SLE, or if he/she is a known SLE patient with worsening symptoms.
LABS
The nurse should be prepared to draw blood specimens for a complete blood count and chemistries, and to obtain a urinalysis, upon order from the provider. They may also order autoimmune tests. Remember that SLE patients are prone to renal problems even when they are not symptomatic, and they typically have abnormalities of the red and white blood cell counts. Other tests may be ordered based upon presenting complaints, such as liver enzyme studies, and amylase and lipase levels.
PATIENT EDUCATION
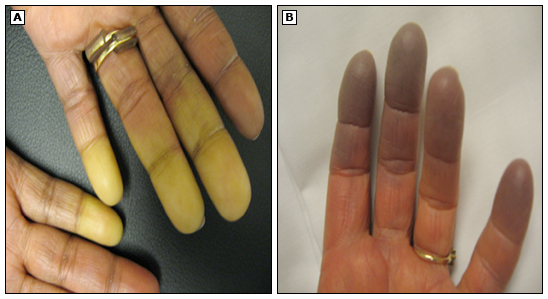
As always, patient education is perhaps the most important thing we do for our patients. For patients who are newly diagnosed, a basic overview of SLE should be shared. Patient education information can be obtained from the Centers for Disease Control and Prevention and the Lupus Foundation of America that may help simplify the important initial pieces of information that the patient needs to know (See Patient Resources at the end of this post). Whether the patient is newly diagnosed, or they have been dealing with the effects of SLE for many years, patient education should be conducted to include strategies to address fatigue; maintenance of a healthy weight; identification of the presence of infection/fever and the importance of notifying healthcare staff; identification of feelings of sadness, depression, anxiety, and coping strategies to address them; the serious photosensitivity of the disease and the importance of sun protection; and keeping warm for those with Raynaud’s Syndrome.
Patients should also be taught how to do gentle stretching exercises for any joint involvement, and the potential for heat to help with stiff joints. In the correctional environment, this may mean a wash cloth soaked with hot water, and then rung out and applied to the joints involved. An exercise program during remission periods is also very important. If an assistive device is necessary, the nurse must ensure that the patient understands how to use it. Medication education should include the name of the drug, the dosage, potential side effects, when to report symptoms to the healthcare staff and any symptoms/condition that should be considered an emergency.
THE CORRECTIONAL ENVIRONMENT
In the correctional environment, SLE patients may need a special diet to address their nutritional status. They may require special housing if they have Raynaud’s Syndrome and the temperature is not able to be regulated easily in the general housing units, or they may require extra blankets, gloves, etc. SLE patients may require special housing if they are immunocompromised. They do require a referral to Mental Health for provision of ongoing support for the psychological effects of the disease. They should be enrolled in the Chronic Disease program and monitored on a routine basis. Pregnant women with SLE are considered high-risk, and should be monitored very closely in the correctional setting.
This series of posts about Systemic Lupus Erythematosus is based upon The Correctional Nurse Educator class entitled Systemic Lupus Erythematosus for the Correctional Nurse.
Please share your experiences caring for patients with Systemic Lupus Erythematosus in our comments section.
Resources
Lupus Foundation of America. https://www.lupus.org
Centers for Disease Control and Prevention. https://www.cdc.gov/lupus/index.htm