Osteoarthritis and Rheumatoid Arthritis are both debilitating diseases that affect millions of individuals in the United States. In the correctional environment, the latest statistics by the Bureau of Justice indicate that “Arthritis” is the third largest chronic diagnosis for jail detainees and is the second largest chronic diagnosis for individuals incarcerated in prisons. Osteoarthritis and Rheumatoid Arthritis are often thought of as the same, but they are different diseases with different etiologies and somewhat different treatments. Today we will be discussing Osteoarthritis.
Osteoarthritis
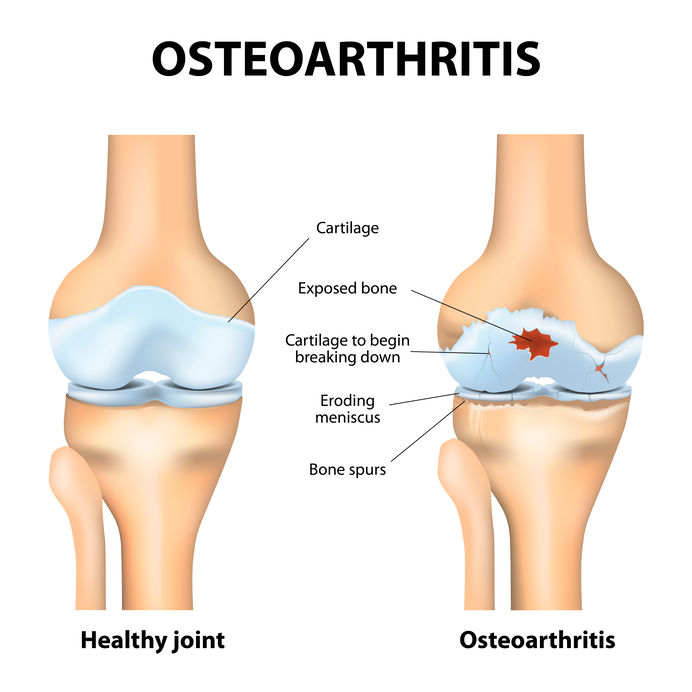
Most often associated with aging and trauma over time to the same area, osteoarthritis (OA) is a progressive disease that affects the moveable joints of the body. In the United States, OA is the most common joint disorder, with more than 30 million individuals afflicted by it. It was previously called degenerative joint disease (DJD), and some patients may still use that name. It is very important to note that OA is not a systemic disease, nor is it associated with inflammation. Typically, the stiffness and discomfort associated with OA improve with moderate use and worsen after extended periods of rest. The most affected joints in the body are the weight-bearing joints – knees, hips, cervical and lumbar spine, and feet. OA causes a loss of cartilage and progressive erosion of the bone. At the same time, bony outgrowths called “spurs” form and expand into the joint. This causes limited and very painful joint movement.
Idiopathic OA, also called primary OA, can occur on one side of the body (unilaterally) in one or more joints and is usually associated with wear and tear of the hand, wrist, hip, and knee joints. More than half of all persons over age 65 have evidence of idiopathic OA. The course of the disease is slow and progressive, without exacerbations and remissions. As the progressive joint deterioration occurs, the joint cartilage has decreased tensile strength and reduced nutrient supply. Patients may experience limitations that range from minor finger discomfort to severe disability of the hip or knee joints. Complications include reduced range of motion, pathological fractures, deformities, immobility, and bone necrosis.
CAUSES OF OSTEOARTHRITIS
There are no known specific causes of OA. While OA was considered a non-inflammatory condition, increasingly experts are finding that inflammatory mediators are released into the joint and surrounding cartilage, bone, and synovial fluid. Aging, obesity, trauma, and familial tendencies have been identified as common risk factors. Additional risk factors include muscle weakness, infection, inflammatory arthritis, Paget disease, joint injuries, bleeding into the joint, joint abnormalities, and excessive joint use such as occurs in occupations like high-impact sports, construction work, and dance. Modifiable risk factors include cigarette smoking, low physical activity, low body weight, estrogen deficiency, alcohol abuse and recurrent falls.
NURSING INTERVENTIONS FOR THE PATIENT WITH OSTEOARTHRITIS
Patient Education
If the patient has had the disease for some time, ask how it has affected his or her life in the free world, and how well he or she is adapting to the correctional environment. What assistance do they need? The patient can be taught assistive techniques to manage joint pain, such as meditation and distraction. They should also be taught gentle range of motion exercises for the affected joint(s). If necessary, the patient can apply moist heat with facecloths/towels to relieve joint pain and to help with the range-of-motion exercises.
Medication
The patients prescribed calcium metabolism modifiers, NSAIDs, and salicylates may need periodic laboratory monitoring of liver and kidney functioning. While the ordering of such testing is the responsibility of the provider, the nurse should expect to obtain the specimens. Patients should be taught common drug interactions for the medications they are prescribed. They should be instructed not to take over-the-counter drugs or change the dosage of prescribed NSAID medications without consulting the healthcare staff. Instructions regarding medication should include the importance of taking medications with food or right after meals to minimize the potential for gastrointestinal discomfort.
Finally, as with all nursing encounters, be sure to document all in the health record, including patient teaching and the patient’s response to any nursing intervention provided.
Information for this blogpost is taken from The Correctional Nurse Educator class entitled Arthritis for the Correctional Nurse.
Please share your experiences caring for arthritis patients in the comments section below.