Abdominal pain is perhaps one of the most frequent complaints listed on a Health Service Request Form in the correctional environment. Changes to routine and diet, stress, and the “unmasking” of symptoms as patients become “detoxed” from substances like alcohol and drugs may contribute to complaints of abdominal problems. It is important that the correctional nurse understand the pathophysiology of the abdomen, and how to conduct a proper assessment of the abdominal areas. As with all presenting complaints, it is vital that a succinct, yet thorough history be obtained from the patient to include any health problems they were experiencing in the past or prior to their incarceration. The myriad of conditions that may present with abdominal pain include gall bladder disease, liver disease, pancreatitis, appendicitis, spleen problems, ulcers, diverticulitis, intestinal obstruction, cancer, ovarian cyst, ectopic pregnancy, GERD, pericarditis, and intestinal gas, just to name a few! While it is not within the scope of practice of correctional nurses (LPNs or RNs) to diagnose the condition of their patient with abdominal pain, it is important that the correctional nurse have a basic understanding of the pathophysiology so that they can determine when a provider needs to be notified.
History
It is important that a thorough history be obtained from the patient. Questions should include whether the patient has/is experiencing nausea or vomiting; and their current bowel and bladder habits, including constipation, diarrhea and any changes to his/her usual bowel and bladder regimens. If the patient is experiencing abdominal pain, the nurse should ascertain its location, duration, intensity, factors that make it worse, and factors that make it better.
- Has the patient’s appetite changed, or has he/she recently gained or lost weight?
- Has the patient experienced bloating, gas, belching, dysphagia, heartburn or indigestion?
- Is he/she complaining of black stools or blood in his/her stool?
- What medications is he/she currently taking? Has the patient started or stopped a medication recently?
- Does he/she have a history of liver problems, to include a known history of liver disease, or intravenous drug use, gall bladder disease, pancreatitis, fever or general malaise?
- Has the patient been diagnosed with HIV, Hepatitis, peptic ulcer disease, GERD, bleeding or platelet disorders?
- Have they had previous abdominal surgery or trauma?
- Are they smokers, caffeine drinkers or alcohol drinkers?
- For female patients, a gynecological history, to include last menses, typical cycle for menses, pregnancies, gynecological surgeries and STI/STD history should be obtained.
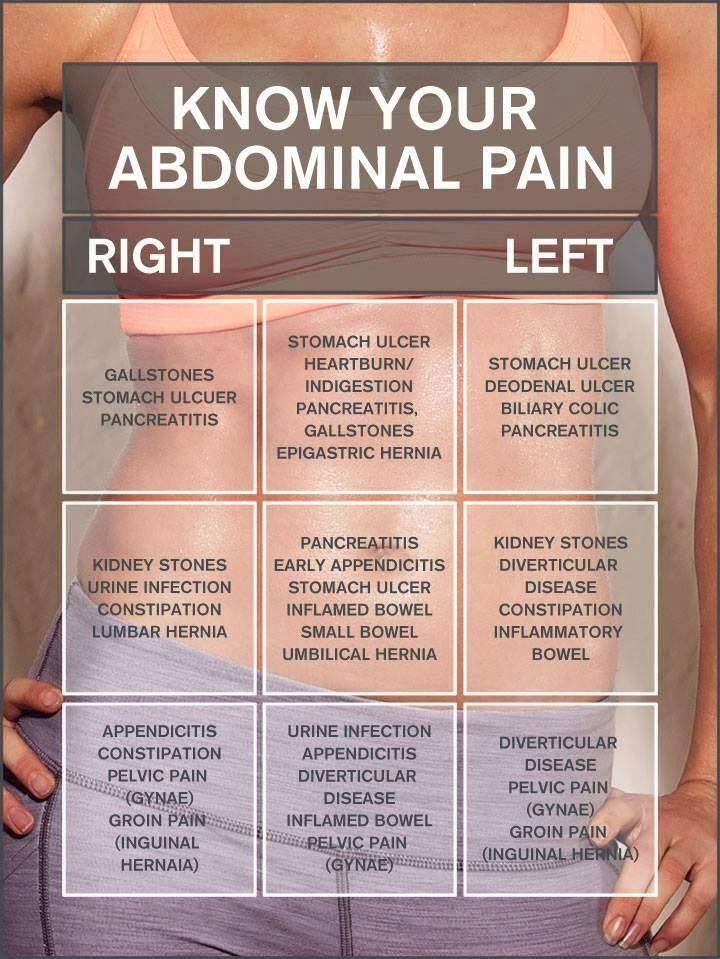
The Abdominal Assessment
The physical examination of the patient begins with inspection. Unique to the sequence of the abdomen, the abdomen is then auscultated, percussed and finally, palpated. Auscultating before the percussion and palpation of the abdomen ensures that the examiner is listening to undisturbed bowel sounds. In addition, if the patient is complaining of pain, leaving the palpation until last allows the examiner to gather other data before potentially causing the patient more discomfort. When completing the physical examination, it is helpful to divide the abdomen into regions in order to consider which organs are involved. A four-quadrant system – left upper quadrant, left lower quadrant, right upper quadrant and right lower quadrant provides a more general overview, and is acceptable in situations when there is no abdominal complaint. The nine-region system provides more specific information if the patient is complaining of discomfort or problems in a certain area. The nine regions include the following: right hypochondriac (upper) region, right lumbar (middle) region, right iliac (lower) region, left hypochondriac (upper) region, left lumbar (middle) region, left iliac (lower) region, epigastric region, umbilical region, and hypogastric (suprapubic) region.
In our next post, we will review the techniques for inspection, auscultation, palpation and percussion and important findings that should be brought to the attention of a provider. What unusual presentation of abdominal pain have you experienced as a correctional nurse?
Leave a Reply