Nursing Assessment of the Asthma Patient
The assessment of a patient with asthma should begin with baseline vital signs, including a pulse oximetry reading. The patient’s lungs should be auscultated, and notation should be made of the patient’s skin color, temperature and moisture. A basic physical examination will also include auscultation of the heart and an abdominal assessment. A baseline peak flow measurement should be obtained. All information should be recorded in the health record. In addition, the patient’s health history should be obtained, including the age at which the asthma diagnosis was made, medications currently taking, known allergens and triggers, last acute exacerbation, past hospitalizations for asthma, past intubations and any other health information pertinent to the patient’s asthma condition, such as other chronic conditions.
When a patient presents with an acute asthma attack, the assessment should be prioritized based upon the patient presentation. The patient should be observed for signs of respiratory distress, including the use of accessory muscles, retractions, purse-lip breathing, and cyanosis of lips/fingers. If the patient is able to communicate, the history of the episode should be ascertained (when did it start, any contact with known triggers, was it progressively worse or immediately bad). The facility policy and procedure will dictate processes to follow, but most likely if the patient is having an acute, severe attack, 911 will be called first. Nursing activities include obtaining vital signs, with pulse oximetry; auscultating all lung fields, noting adventitious sounds and locations; obtaining peak flow measurements; and contacting the Provider for orders. A breathing treatment or administration of medication via a metered dose inhaler should be an expected order, and the nurse should be ready to administer this immediately when the order is obtained. If the provider has previously seen the patient in Chronic Disease Clinic (or even in Provider Sick Call), the Provider may have already ordered as needed nebulizer treatments/rescue inhaler use for the patient, in which case nursing staff may administer it immediately. Remember to measure peak flow before and after the treatment, if the patient’s condition allows. Once the treatment is completed, continue to monitor the patient for a time in the health unit to ensure that they will not have a rebound attack. Most often, even if you did not have to contact the provider for the treatment order, you should contact the Provider after the treatment to report the patient’s presentation and condition post-treatment, so that an appropriate treatment plan can be developed.
Patient Education For the Asthma Patient
Patient education for the asthmatic patient should include the following:
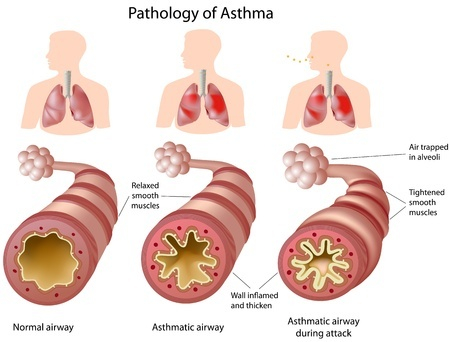
Basic facts about asthma – The contrast between airways of a person who has and a person who does not have asthma; the role of inflammation and what happens to the airways during an asthma attack.
Trigger avoidance – This seems so obvious, but may help the most in asthma management.
Role of Medication – Quick-relief medications: Short-acting beta2 agonists (SABAs) relax airway muscles to provide prompt relief of symptoms. Do not expect them to provide long-term asthma control. Using SABA >2 days a week indicates the need for starting or increasing long- term control medications.
Role of Medication – Long-term control medications: Must be taken daily. They prevent symptoms, often by reducing inflammation. Do not expect them to give quick relief.
Review of the Asthma Action Plan with the patient to ensure understanding after it has been developed by the Provider/Chronic Care Nurse in partnership with the patient.
Encourage patient self-monitoring, including the self-assessment of asthma control and the identification of symptoms of worsening asthma, and the importance of reporting all changes to nursing staff.
Encourage hydration, as this helps thin secretions and mucous.
If the site has a SAM/KOP program, ensure that patient understands the importance of informing the nurse about their rescue inhaler usage before it becomes problematic.
Smoking cessation. Most facilities are smoke-free, and incarceration is a great time for patients to begin their smoking cessation. For those that have e-cigarettes available, remember to educate that they are still inhaling chemicals into their lungs!
This post is based upon The Correctional Nurse Educator classes Asthma I and II for the Correctional Nurse.
Please share any pearls you have for patient education for the Asthma patient in our comments section.