One of the first things I discovered when I entered correctional nursing was how little I knew about dental issues or conditions. I must have daydreamed through this section of nursing school, or maybe we just didn’t give enough attention to oral assessment and dental emergencies. In any case, correctional nurses need to understand dental conditions as we are often the ones to determine if a patient needs to see a dentist urgently or at the next available opening.
Nurses in jails and prisons must assess for, manage or defer dental issues or conditions as a part of daily practice. The inmate population, as a rule, has not had regular dental care so things can really look bad in there. Dr. Stephen Mitchell, a correctional dentist from Atlanta, GA and Director of Dental Services for CorrectHealth, shared some common inmate dental conditions at the recent ACHSA national conference. Here are some key points from his session.

Dental Issues for Correctional Nurses
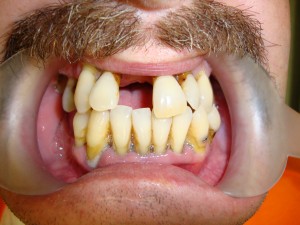 Tooth sensitivity and bleeding from gingivitis or periodontitis may not been felt or considered by the inmate until they have withdrawn from their drugs and alcohol from the street. Once off their self-medication, dental discomforts can become a concern. Although the patient may suggest otherwise, these conditions did not appear overnights but likely were developing for some time, just not noticed. For example, poor oral hygiene can lead to such extensive tartar build-up that the teeth can chip and break requiring removal (pictured at the left). Gingivitis, periodontitis and excessive tartar are not emergencies but will affect eating and require dental services.
Tooth sensitivity and bleeding from gingivitis or periodontitis may not been felt or considered by the inmate until they have withdrawn from their drugs and alcohol from the street. Once off their self-medication, dental discomforts can become a concern. Although the patient may suggest otherwise, these conditions did not appear overnights but likely were developing for some time, just not noticed. For example, poor oral hygiene can lead to such extensive tartar build-up that the teeth can chip and break requiring removal (pictured at the left). Gingivitis, periodontitis and excessive tartar are not emergencies but will affect eating and require dental services.
Mouth ulcers can also develop and are not emergencies. Dr. Mitchell suggested treatment with a simple salt water gargle. He suggests directing the inmate to use a salt packet from the chow-line in a cup of water. Ulcer can develop from ill-fitting dentures. A dental visit is required to evaluate need for resurfacing the dentures, in this case.
Bacterial tooth infection can irritate the tooth pulp and cause an abscess. Pain and swelling shows that infection is present. In this case, antibiotic treatment is needed short term. Long term treatment may require tooth removal or root canal. Root canals are not frequently done in jails. An extensive abscess may cause the face to look swollen on the affected side. It is important that the infection does not spread to the airway or eye socket. The condition should be treated before it spreads. An abscess, unlike other conditions, is going to be very tender and soft. The tooth may not appear defective. Facial trauma can result in tooth nerve death and lead to an abscess.
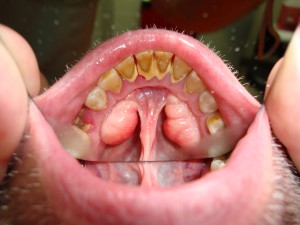 A condition of bony growth, called dental tori (pictured at the left), can mimic abscess but is really benign and requires no treatment. When assessing for abscess, be sure that the growth or swelling is red, soft, and tender. Dental tori are a natural color (if not irritated), firm, and non-tender.
A condition of bony growth, called dental tori (pictured at the left), can mimic abscess but is really benign and requires no treatment. When assessing for abscess, be sure that the growth or swelling is red, soft, and tender. Dental tori are a natural color (if not irritated), firm, and non-tender.
Pericoronitis is also common in the inmate population. This condition may present as an abscess but really results from an unerrupted wisdom tooth. Gum tissue overgrowth can get in the way of chewing and become swollen and sore. Antibiotics will reduce swelling, if extensive. Otherwise, good oral hygiene – regular brushing, flossing and debris removal – will improve this condition.
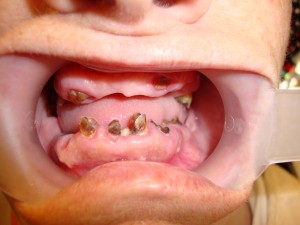 Meth mouth (pictured at the left) is a dental condition brought on by chronic meth drug use. It involves accelerated tooth decay and loss. The intense decay can appear an emergency requiring immediate treatment. However, this is rarely necessary. The condition is caused by the loss of saliva and increased intake of sugar. Generally the mouth does not feel painful to the patient. This decay happens quickly in 1-2 years of meth use. Long term meth use leads to further damage and tooth loss. Sometimes teeth break off at the gum line.
Meth mouth (pictured at the left) is a dental condition brought on by chronic meth drug use. It involves accelerated tooth decay and loss. The intense decay can appear an emergency requiring immediate treatment. However, this is rarely necessary. The condition is caused by the loss of saliva and increased intake of sugar. Generally the mouth does not feel painful to the patient. This decay happens quickly in 1-2 years of meth use. Long term meth use leads to further damage and tooth loss. Sometimes teeth break off at the gum line.
Cataloging all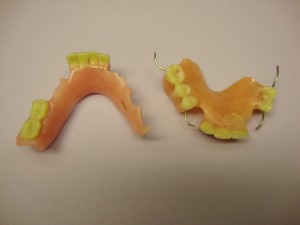 tooth equipment on intake is an important nursing function. This helps validate patient information later in the stay. For example, a patient might contend that a dental partial plate was taken from them during a cell sweep. This might be an expensive replacement. However, careful documentation on intake might reveal that the patient did not enter the facility with their partial. It can also be important to document any broken teeth on intake. Reports from an inmate that they broke their tooth falling in their cell can be validated.
tooth equipment on intake is an important nursing function. This helps validate patient information later in the stay. For example, a patient might contend that a dental partial plate was taken from them during a cell sweep. This might be an expensive replacement. However, careful documentation on intake might reveal that the patient did not enter the facility with their partial. It can also be important to document any broken teeth on intake. Reports from an inmate that they broke their tooth falling in their cell can be validated.
Understanding dental terminology will speed documentation and keep communication clear. Dr. Mitchel clarified the following dental terms for use in charting
- Bridges don’t leave the mouth. These are permanent and connect several teeth together for support.
- Partials (pictured at the left) are removable and often involve metal work to anchor them in the mouth. They are expensive to create and replace. Inmates may have a less-expensive temporary partial, sometimes called a flipper. Temporary partials solve the issue of missing teeth without extensive fitting. Temporary partials have much less metal and crafting. Documenting that a partial is a temporary can be very helpful should the item be lost or destroyed during incarceration.
- Dentures are solid castings of the full upper or lower set of teeth.
- Inmates may arrive at the facility with orthodontic wires. Standard braces are found in the middle of the teeth and are used to straighten teeth. Arch bars are found below the gum line and are placed temporarily for bone healing after facial trauma. Normally, arch bars are removed after 6-8 weeks, but since this usually involves an office visit and expense, many inmates do not return for removal. Arch bars can remain in the mouth. It is not required that they be removed during incarceration.
By focusing on oral assessment and developing an understanding of common and emergent dental conditions, you can solve the mystery of inmate dental conditions. Share your dental stories in the comments section of this post.
Photo Credit: © dragon_fang – Fotolia.com Dental images courtesy of Stephen Mitchell
Leave a Reply