Rhabdomyolysis means the “dissolution of skeletal muscle”. It is a syndrome caused by direct muscle injury, or a mismatch between energy production and energy consumption that results in a breakdown of muscle cells. This breakdown results in the leakage of potentially toxic intracellular contents into the systemic circulation. While there are many causes for rhabdomyolysis, the most common include trauma, drugs/alcohol, and strenuous exercise. The classic symptoms of rhabdomyolysis include a triad of muscle weakness, myalgia, and dark urine. It was initially described in the victims of crush injury during World War II, and was called the Meyer Betz disease. Management of rhabdomyolysis consists primarily of the correction of fluid and electrolyte abnormalities. It may be managed onsite if the damage is mild, but most often these patients will be sent to the emergency department. Nursing interventions include obtaining ordered lab tests, hydration, patient monitoring and patient education.
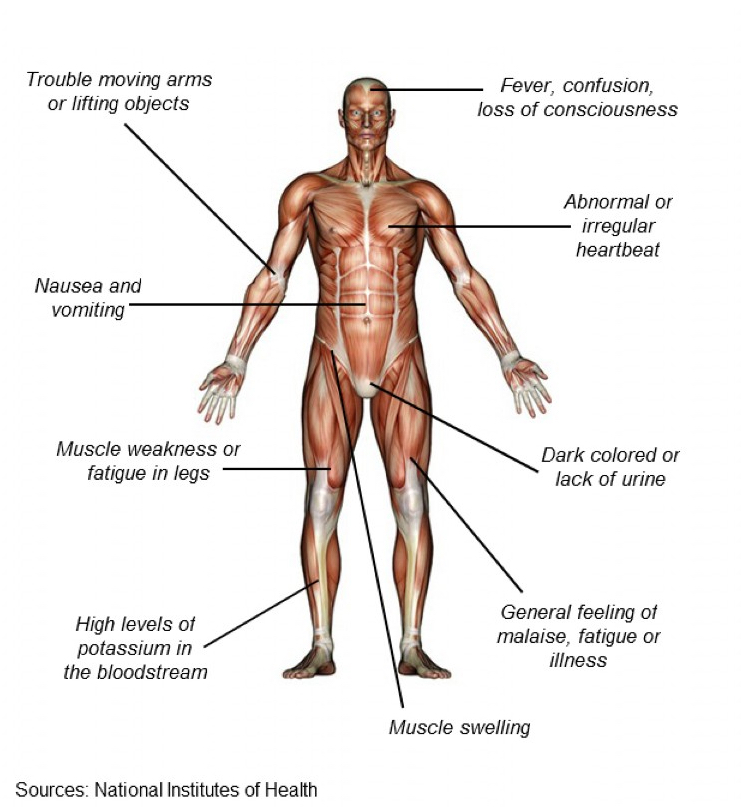
The signs and symptoms of rhabdomyolysis
Rhabdomyolysis may be caused by a number of conditions and factors, including trauma; muscle compression; infection from bacteria; viruses and fungi; conditions that impair the metabolism of the muscle fibers, genetic conditions that impair the muscle metabolism; drug use (illicit, prescription and over the counter); and exertional physical activity that overloads the system. In the correctional environment, we most often see rhabdomyolysis as a result of exertional activity and substance use, to include drugs that increase cell energy requirements, like methamphetamine, MDMA and cocaine, and alcohol abuse that causes metabolic abnormalities through both direct toxicity and the disruption of the muscle blood supply due to immobilization. Interestingly, research has indicated that other “common” drugs that may result in rhabdomyolysis include antihistamines, statins, salicylates, antipsychotics, SSRIs, antidepressants, corticosteroids, colchicine and protease inhibitors. This means that if you have a patient prescribed an antipsychotic and they start to engage in an exercise program, and then submit a sick call slip for general weakness, nausea and muscle aches, they need a complete physical assessment and most likely an evaluation by a provider.
There are four stages of Rhabdomyolysis
STAGE ONE
Stage one is the primary injury. This could be a motor vehicle accident which causes direct muscle injury, although there are other ways in which this disease can begin. Muscle compression during an overdose can also cause primary injury, as can immobilization due to alcohol intoxication and “passing out”. The other principle cause occurs when the energy supply to a muscle runs out, for example during a tonic-clonic seizure, or during a marathon when the body has exhausted its energy supply and muscle starts to break down. In the correctional environment, we often see individuals who had not been previously athletic, but who now have time and begin a vigorous exercise program. At this stage, the patient may have few symptoms, and they are mostly generalized, such as fatigue, muscle aches and slight edema.
STAGE TWO
In stage two, normal muscle cell function is disrupted. Energy for cellular function is normally derived through aerobic (where glucose is broken down into CO2 and H2O giving rise to energy) or anaerobic (glycolysis) cellular metabolism. Failure of this process leads to muscle cells leaking electrolytes such as potassium and phosphates into the blood supply, while allowing the entry of calcium, sodium and water into the cell from the blood supply. At this stage, the patient may have generalized symptoms, or may have already progressed to severe pain, gross edema and even confusion.
STAGE THREE
In stage three, the side effects of this disruption can be seen as the muscle cells swell due to increased water uptake. Together with the resulting interstitial edema, the patient develops third spacing, and hypovolemia. The resulting damage to the cell leads to further functional impairment at the cellular level, ultimately leading to cell death. During this time, the intracellular contents leak into the blood stream causing systemic disruption. At this stage, the correctional patient most often exhibits a multitude of significant signs and symptoms and should be sent to the emergency department.
STAGE FOUR
Stage four is the final stage of the cascade, when the muscle cell death and systemic complications may lead to renal dysfunction. The patient at this stage should be hospitalized, as they may need systemic support and dialysis.
In our next post, we will discuss the evaluation of the patient presenting with signs of rhabdomyolysis, including the subjective questions to ask and the objective assessment to perform.
This post is based on The Correctional Nurse Educator class Rhabdomyolysis for the Correctional Nurse.
Please share your experiences with rhabdomyolysis in the correctional environment in our comments section.
Leave a Reply