A young woman in custody at a large urban jail had continuing abdominal pain over a 14 hour period. She was found unresponsive in her cell and rushed to the hospital where she was pronounced dead on arrival. Autopsy revealed a ruptured ectopic pregnancy. What assessments and testing should have been done for this woman?
The word “ectopic” means out of place. Ectopic pregnancy, where a fertilized ovum implants somewhere outside the uterus, is an emergency event every correctional nurse should consider when presented with abdominal pain in a female patient of reproductive age. This condition is especially common among women with a history of sexually transmitted infections, Pelvic Inflammatory Disease (PID), previous ectopic pregnancy, previous abdominal surgery or infertility. Smoking also increases risk. These are all characteristics that are common in the female incarcerated population.
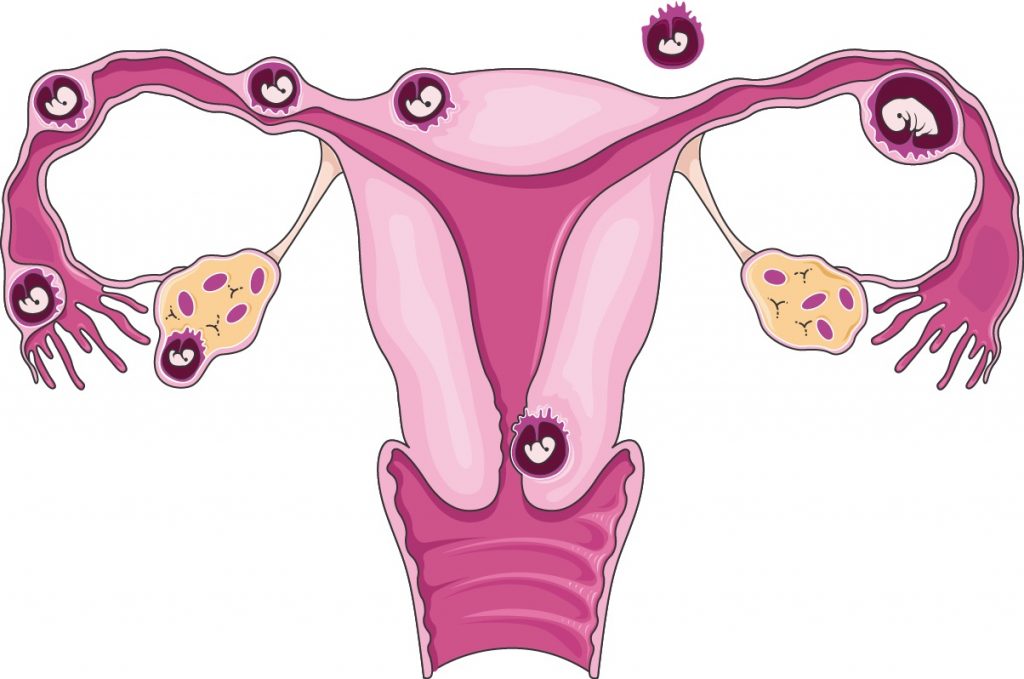
Potential causes of acute pelvic pain in women
- Appendicitis
- Ectopic Pregnancy
- Endometriosis
- Ovarian Cyst or Torsion
- Pelvic Inflammatory Disease
- Diverticulitis
- Kidney/Urethral stone
- Hernia
Signs and Symptoms
Ectopic pregnancy is heralded by the following three symptoms: abdominal pain, amenorrhea and vaginal bleeding. However, research has shown that only about 50% of patients present with all three symptoms. Patients may also present with other signs and symptoms of early pregnancy, such as nausea and breast fullness. Patients may report dizziness, weakness and syncope; fever; flu-like symptoms; and vomiting. As the pregnancy advances, symptoms worsen.
Patients with an ectopic pregnancy can become unstable quickly. If a tubal rupture takes place, the pain will intensify and signs of shock such as low blood pressure and a rapid thready pulse will be evident. Intraperitoneal hemorrhage can cause referred pain to the shoulder area and a very tender abdomen.
Patients who present with abdominal rigidity, involuntary guarding, severe tenderness, orthostatic changes to vital signs and tachycardia should be sent emergently to the closest hospital, as the presence of these symptoms suggest a surgical emergency.
Serum β-HCG levels
In a normal pregnancy, the β-HCG level doubles every 48-72 hours until it reaches 10,000-20,000mIU/mL. In ectopic pregnancies, β-HCG levels usually increase less. Average serum β-HCG levels are lower in ectopic pregnancies than in healthy pregnancies.
No single serum β-HCG level is diagnostic for an ectopic pregnancy. Serial serum β-HCG levels are necessary to differentiate between normal and abnormal pregnancies, and to monitor the success of the therapeutic intervention to eliminate the ectopic pregnancy.
Ultrasound
Ultrasonography is probably the most important tool for diagnosing an ectopic pregnancy. Visualization of an intrauterine sac, with or without fetal cardiac activity, is often adequate to exclude ectopic pregnancy.
Nursing Interventions
Ectopic pregnancy is a medical emergency requiring fast action. Shock and death can follow quickly and immediate stabilization and transport to emergency treatment are necessary. Nursing staff should seek immediate medical evaluation for any potentially pregnant patient with unexplained abdominal pain. Be ready to initiate emergency protocols, which can include establishing intravenous access and administering fluids per provider order. Ruptured ectopic pregnancy is the leading cause of maternal mortality in the first trimester and research indicates that it results in 4% of all maternal deaths.
Patient counseling and support are perhaps the most important nursing intervention for the patient with an ectopic pregnancy once stabilized. It is a medical emergency, and keeping the patient calm and informed is very important. Medication per provider order and monitoring the patient to ensure safety until she is transported are also critical nursing functions. Patient education should include the reason for use, mechanism of action, dosage, and potential adverse effects of all prescribed medications. Patent education with regard to expectations of activities that will occur when she gets to the hospital is also very helpful and often decreases the level of anxiety of the patient.
Upon return to the facility, monitoring and patient education regarding her treatment plan and expected course of recovery should be done. Watch for signs of depression! As always, documentation of the nursing interventions and the patient’s response, as well as updating the treatment plan to reflect changes in the patient’s condition is of upmost importance.
Have you had an experience with an ectopic pregnancy in a jail or prison setting? Tell us your story in the comments section of this post.
Materials contributing to this post include information from The Correctional Nurse Educator class – Abdominal Assessment for the Correctional Nurse: Lower Abdominal Pain.
Leave a Reply