One in ten doctors and NURSES abuse drugs or alcohol. Is this surprising to you? It was to me when…
Read More
Nursing Practice
Correctional Nurse Practice Update: Four Ways to Build a Trust Relationship with Incarcerated Patients
Correctional nurses must quickly develop a trust relationship with their patients in order to collect accurate data and effectively evaluate…
Read More
Correctional Nurse Professional Update: Moral Distress, When Doing the Right Thing Feels Out of Reach
Correctional nurses are often called upon to balance their professional duty with the realities of a secure environment. This can…
Read More
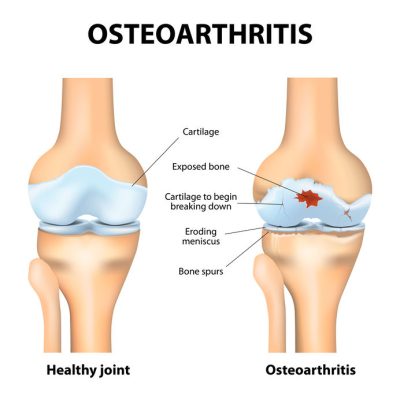
Correctional Nurse Clinical Update: Osteoarthritis
Osteoarthritis and Rheumatoid Arthritis are both debilitating diseases that affect millions of individuals in the United States. In the correctional environment,…
Read More
Correctional Nurse Clinical Practice Update: Arthritis Management Behind the Wall
Arthritis is one of the top five chronic conditions found among our patient population, yet managing this debilitating condition is…
Read More
Correctional Nurse Professional Update: Implicit Bias – Recognizing What We Don’t See
Correctional nurses pride themselves on objectivity, fairness, and professionalism. Yet like all humans, we carry unconscious assumptions that can influence…
Read More